For multispecialty and corporate hospitals, bed availability is not just an operational issue, it directly affects patient experience, emergency responsiveness, staff coordination, and revenue flow. When admissions, discharges, ICU movement, and housekeeping updates are handled through fragmented systems, hospitals often face delayed bed assignments, crowded emergency rooms, and poor visibility across departments.
This is where AI bed management systems can create measurable value. Instead of relying only on manual coordination or static dashboards, hospitals can use AI to support real-time bed availability monitoring, predict occupancy patterns, improve patient movement, and streamline decisions across wards, ICUs, and emergency departments. For hospital leaders in Ahmedabad and other fast-growing healthcare markets, this approach can help turn bed management from a reactive task into a more intelligent operational function.
Operational Challenge
Hospitals rarely struggle because they do not have beds at all. More often, they struggle because they do not have a clear, real-time picture of which beds are available, which will be released soon, and where bottlenecks are forming.
In many facilities, bed status updates move slowly between nursing teams, admission desks, discharge coordinators, transport staff, and housekeeping. A patient may be medically ready for transfer, but the receiving unit may not know it in time. A bed may be cleaned but not marked available quickly enough. Emergency departments may continue holding patients because inpatient units cannot coordinate fast enough. This affects hospital capacity optimization at every level.
These delays can create several practical issues:
- Longer patient wait times in emergency rooms
- Slower admissions from OPD or referral channels
- Poor visibility into ICU and ward capacity
- Inefficient staff workload distribution
- Missed opportunities for faster bed turnover
- Higher administrative pressure during peak demand periods
For administrators focused on patient flow optimization in hospitals, the core challenge is not only tracking beds, but understanding how occupancy changes throughout the day and how decisions can be improved before delays escalate.
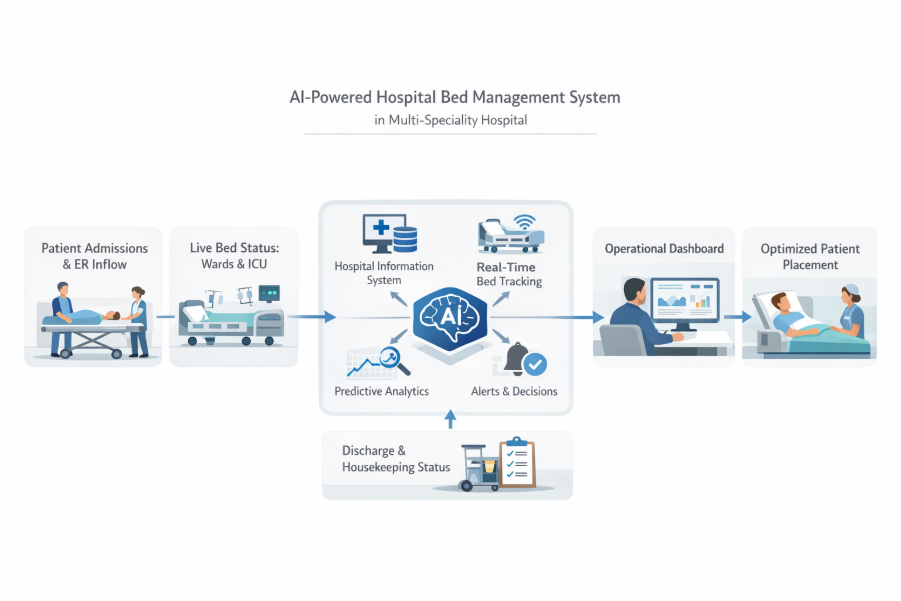
Fig: A conceptual workflow of an AI-Powered Hospital Bed Management System, illustrating how real-time data integration and predictive analytics optimize patient placement from admission to discharge.
How the Solution Can Be Implemented
A practical implementation of AI hospital bed management usually starts with creating a connected view of bed status across departments. The goal is to unify occupancy, discharge planning, housekeeping updates, transfer requests, and admission priorities into one intelligent workflow.
A typical implementation can follow this path:
1. Connect existing hospital data sources
The first step is to integrate the hospital information system, admission-discharge-transfer records, EHR modules, housekeeping updates, and nursing station inputs into a unified data layer.
In modern hospital environments, this integration is typically achieved using interoperability standards such as HL7 and FHIR, which allow different systems to exchange patient and operational data securely and in real time.
This standardized integration is critical for enabling accurate real-time bed tracking and ensuring that all departments operate on a single source of truth.
2. Standardize bed status logic
Hospitals often use inconsistent definitions such as occupied, blocked, reserved, cleaning in progress, ready for admission, or under maintenance. AI models work better when these operational states are standardized across the hospital network.
3. Add real-time monitoring
A real-time bed tracking system can continuously reflect current status by ward, specialty, room type, and critical care category. When supported by workflow automation, updates can move faster and reduce dependency on repeated phone calls or manual follow-ups.
4. Apply predictive logic
AI can analyze historical admissions, average length of stay, transfer patterns, discharge timing, and peak emergency inflow periods. This helps generate bed occupancy forecasting insights so teams can prepare before pressure builds.
5. Automate prioritization and alerts
The system can notify relevant teams when a bed is likely to become available, when an ICU bottleneck is forming, or when the emergency department is approaching overflow. This supports faster response without forcing staff to manually monitor every movement.
6. Use a centralized dashboard for action
A live command-style dashboard can give administrators, operations managers, and unit supervisors a clear view of current capacity, pending discharges, blocked beds, and patient placement priorities. This is where AI-driven healthcare operations solutions become operationally useful rather than theoretical.
Key Capabilities
For hospitals evaluating AI solutions for patient flow management, the most useful capabilities usually include operational intelligence, predictive visibility, and workflow coordination.
Real-time bed visibility
A centralized system can display bed status across departments, floors, special units, and partner hospitals in a network. This reduces communication gaps and improves response speed.
Predictive bed release estimation
AI can estimate when beds may become available based on discharge behavior, procedure completion, transfer timing, and historical patient flow trends. This supports better planning for admissions and transfers.
Smart bed allocation support
Instead of assigning beds only by current vacancy, AI can support better matching based on care level, patient condition, specialty needs, infection control rules, and likely discharge timelines.
ER and ICU pressure alerts
For emergency room efficiency and ICU capacity management, early alerts matter. AI can identify patterns that suggest crowding risk and notify teams before the situation becomes critical.
Workflow automation
Tasks such as discharge-triggered housekeeping requests, transfer coordination, and escalation alerts can be automated. This supports hospital workflow automation and reduces delays between one process step and the next.
Capacity forecasting and reporting
Leadership teams can use predictive dashboards for daily planning, weekend surge preparation, seasonal load management, and executive reporting. This adds value beyond bedside operations.
Technology Stack
A successful deployment does not require hospitals to replace everything. In most cases, the right approach is to integrate with current systems and build a focused intelligence layer on top.
A practical stack may include:
- Hospital Information System and EHR integration
- Admission, discharge, and transfer data connectors
- Mobile interfaces for nursing staff and housekeeping teams
- IoT or occupancy signal integrations where available
- Cloud-based analytics engine for real-time processing
- AI models for discharge prediction and occupancy trends
- Central operational dashboards for supervisors and leadership
- Role-based alerts via web, mobile, SMS, or internal messaging
From a workflow perspective, hospitals can start small. For example, one corporate hospital in Ahmedabad could begin with general wards and emergency admissions, then expand into ICU, surgery recovery, and multi-branch coordination later. This phased approach reduces risk and makes adoption easier.
For organizations exploring AI for hospital capacity planning systems, the architecture should also support audit trails, role-based access control, and scalable integrations so the system remains useful as operations grow.
Business Benefits
The value of AI bed management systems becomes clearer when hospitals measure outcomes in operational terms.
A well-implemented solution can help hospitals:
- Reduce avoidable ER boarding time
- Improve admission-to-bed assignment speed
- Increase bed turnover efficiency
- Strengthen hospital resource utilization
- Reduce manual coordination load for staff
- Improve forecasting for high-demand periods
- Support better executive decision-making
In practical terms, hospitals that improve visibility and automate allocation logic can see measurable gains in throughput and coordination. Early benchmarks suggest that hospitals can target a 30 to 40 percent improvement in resource utilization and patient flow efficiency, particularly when data systems are well-integrated and workflows are consistently followed.
However, actual outcomes may vary depending on factors such as existing digital maturity, staff adoption, data quality, and process alignment across departments.
Compliance Considerations
Healthcare technology decisions must balance operational efficiency with data security, regulatory compliance, and system reliability. Since bed management systems interact with patient-linked operational data, governance becomes a critical factor.
Key considerations include:
- Compliance with India’s Digital Personal Data Protection (DPDP) Act, ensuring secure handling of patient-related data
- Alignment with global standards such as ISO 27001 for information security management
- Role-based access control to limit data visibility across departments
- Secure APIs and encrypted data exchange between HIS, EHR, and analytics layers
- Transparent AI-driven decision support to avoid black-box recommendations
- Audit trails for every bed allocation, discharge update, and system-triggered action
- Clear fallback workflows to maintain operations during system downtime
Beyond compliance, adoption depends on trust. Hospitals must ensure that staff understand and rely on the system, which requires structured training, phased rollout, and continuous process alignment.
Real-World Example
Consider a multi-speciality hospital in Ahmedabad with high emergency inflow and frequent delays in inpatient bed assignment. The hospital uses separate systems for admissions, housekeeping, and discharge coordination. During peak hours, the emergency team often waits for manual confirmation from wards before moving patients.
By implementing an AI-enabled bed management layer, the hospital can unify live bed status, pending discharge signals, cleaning turnaround, and unit-level occupancy dashboards. The platform can estimate likely bed release times, trigger housekeeping automatically after discharge confirmation, and alert administrators when ICU or emergency pressure begins rising.
In this kind of scenario, the hospital can reduce waiting time for admissions, improve coordination between departments, and make faster operational decisions without adding unnecessary administrative burden. This is also a strong example of how hospitals manage bed occupancy efficiently when real-time data and predictive logic work together.
FAQs
- What is an AI bed management system?
An AI bed management system is a hospital operations platform that uses real-time data, automation, and predictive analytics to improve bed allocation, discharge coordination, and patient flow.
- How can AI reduce ER waiting time in hospitals?
AI can reduce ER delays by identifying upcoming bed availability faster, improving transfer coordination, and alerting teams when capacity bottlenecks are likely to occur.
- Can AI help with ICU capacity management?
Yes. AI can support ICU capacity planning by tracking live occupancy, predicting likely discharges or transfers, and helping administrators respond earlier to bed shortages.
- What data is needed for AI hospital bed management?
Most systems use admission, discharge, transfer, bed status, housekeeping updates, and patient flow data. Some hospitals also add IoT signals or live occupancy feeds where available.
- Is AI hospital bed management only useful for large hospitals?
No. Large hospital networks may see broader benefits, but single hospitals can also gain value by improving real-time visibility, reducing manual coordination, and planning bed turnover better.
- What are the main benefits of AI for hospital capacity planning systems?
The main benefits include better bed utilization, improved patient flow, faster admissions, reduced operational inefficiencies, and more accurate occupancy forecasting.
- How should hospitals start implementing AI-driven bed management?
A practical starting point is to connect current systems, standardize bed status definitions, launch a centralized dashboard, and roll out predictive features in phases across departments.
Conclusion
Hospitals do not need more complexity in bed operations, they need better visibility, faster coordination, and smarter planning. That is exactly where AI bed management systems can help. By combining real-time tracking, automated allocation support, and predictive insights, hospitals can reduce avoidable delays, improve bed turnover, strengthen ICU and ER coordination, and build a more reliable operational model.
For healthcare providers looking to modernize patient flow and capacity management, the opportunity is not only technological. It is strategic. A well-designed implementation can support better care delivery, stronger operational control, and higher resource efficiency across departments. For organizations seeking a trusted AI development company in Ahmedabad, the right technology partner should be able to connect AI, Web, Mobile, and Cloud capabilities into a secure, practical hospital operations solution.
Talk to us
If your hospital is exploring smarter ways to improve patient flow, reduce bed allocation delays, or build a more responsive capacity management system, Theta Technolabs can help you design and implement the right solution.
Our team delivers AI-driven healthcare platforms backed by web, mobile, and cloud expertise, helping hospitals build practical systems for real-time monitoring, workflow automation, and predictive operational intelligence.
To discuss your hospital operations use case, reach out at sales@thetatechnolabs.com.

















_Computer%20Vision-enabled%20Web%20and%20Mobile%20Interfaces%20for%20Mall%20Management%20in%20Dubai_Q1_In_24.avif)
_Smart%20Solutions%20for%20Healthcare_%20How%20IoT%20Development%20is%20Reshaping%20Dubai%20Hospitals_Q1_In_24.avif)
_Automated%20Checkout%20Systems.avif)
_Smart%20Manufacturing%20in%20Dubai_%20How%20AI%20is%20Driving%20Efficiency%20and%20Innovation_Q1_In_24.avif)

_Understanding%20the%20Impact%20of%20AI%20and%20Machine%20Learning%20on%20Fintech%20Web%20Apps%20in%20Dubai_Q2_24.avif)
_Explore%20the%20Best%20Cross-Platform%20App%20Development%20Frameworks%20of%202024_Q3_24.avif)


_Top%20Benefits%20of%20Cloud%20Computing%20for%20All%20Business%20Sectors_Q2_24.avif)
_Integrating%20IoT%20with%20Mobile%20Apps%20for%20Advanced%20Renewable%20Energy%20Solutions_Q2_24.avif)


_The%20Transformative%20Role%20of%20Open%20Banking%20APIs%20in%20Fintech%20for%202024_Q3_24.avif)
_Choosing%20the%20Right%20Computer%20Vision%20Development%20Partner%20in%20Ahmedabad%20for%20Construction_Q3_24.avif)
_Node.js%20and%20Blockchain_%20A%20Perfect%20Pair%20for%20Fintech%20Innovation%20in%20Dubai_Q3_24.avif)
_How%20AI%20Development%20Companies%20in%20Ahmedabad%20are%20Transforming%20the%20Shopping%20Experience_Q4_25.avif)
_How%20IoT%20Can%20Reduce%20Energy%20Costs%20in%20Smart%20Factories_Q4_25.avif)























.avif)
.avif)
.avif)


































.png)




.png)

















