In 2026, healthcare systems are no longer judged only by how well they respond to illness. They are evaluated on how effectively they anticipate it. Clinical leaders today face a reality where patient volumes are rising, chronic conditions are more complex, and staffing constraints are persistent. At the same time, expectations from patients, regulators, and payers have never been higher.
Now imagine a different operational model. What if your hospital could identify patient deterioration days earlier, adjust care plans in real time, and support clinicians with data-backed foresight rather than alerts after the fact? This is the promise of ai-driven predictive care in healthcare, not as an experimental technology, but as a strategic intelligence layer embedded across clinical and operational workflows.
From Detecting to Forecasting: The Shift That Redefines Care Delivery
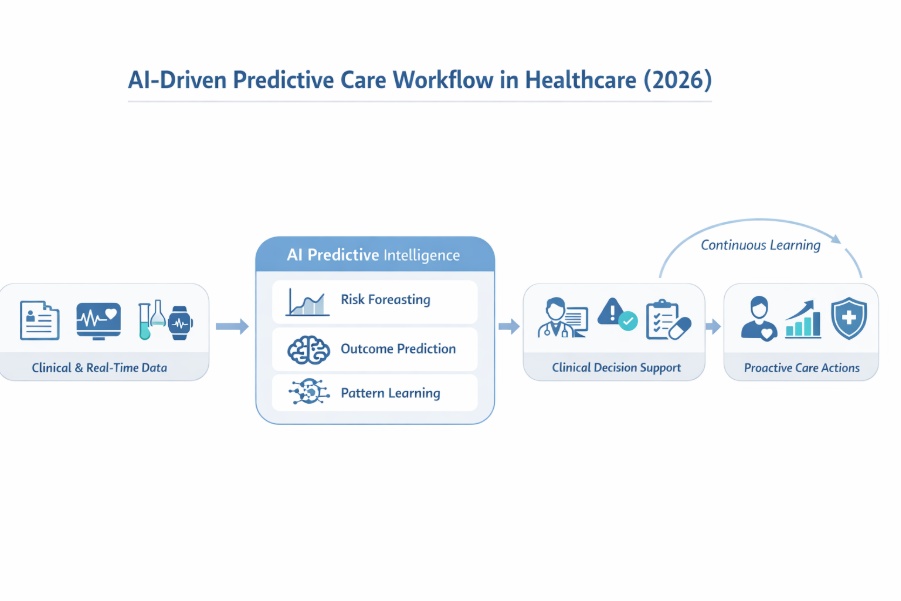
Traditional healthcare analytics focused on detection. A lab result flags abnormal values. A monitoring system triggers an alert when vitals cross a threshold. These tools are valuable, but they operate after risk has already materialized.
In contrast, ai-driven predictive care in healthcare is built around forecasting. By continuously analyzing longitudinal patient data, real-time physiological signals, and historical outcomes, AI models identify patterns that humans cannot easily see. The result is risk prediction that looks forward, not backward.
In 2026, this shift is powered by agentic AI systems. These systems do more than generate predictions. They coordinate actions across clinical decision support platforms, care management tools, and operational systems. For example, instead of notifying a nurse about an abnormal heart rate, the system forecasts the likelihood of cardiac instability within the next 48 hours and recommends preventive interventions.
This forecasting capability fundamentally changes how care teams operate. Clinical decisions are no longer reactive responses to events. They become proactive strategies guided by probability and context.
Transforming the Patient Journey with AI-Based Patient Outcome Forecasting
What if every patient journey was continuously optimized based on predicted outcomes rather than standardized pathways?
AI-based patient outcome forecasting enables exactly that. These models assess how individual patients are likely to respond to treatments based on factors such as comorbidities, lifestyle indicators, genomic data, and prior clinical history. The result is care personalization at scale.
In a predictive care environment, early diagnosis becomes more precise. Subtle deviations in lab trends or wearable data can signal disease onset before symptoms are clinically obvious. For chronic patients, AI systems adjust care plans dynamically, reducing unnecessary interventions while escalating support for high-risk individuals.
From a patient perspective, this translates into fewer emergency admissions, shorter hospital stays, and care that feels tailored rather than generic. From a clinical perspective, it means higher confidence in treatment decisions supported by continuously learning models.
Operational Efficiency: How Healthcare Predictive Analytics Reduces Burnout
Clinician burnout remains one of the most critical challenges in 2026. Documentation overload, alert fatigue, and administrative friction continue to drain time and focus from patient care.
This is where healthcare predictive analytics plays a transformative role. Instead of generating more alerts, predictive systems prioritize information. They surface only the risks that matter most, at the moment when intervention has the highest impact.
AI-driven workflows also support automated prior authorizations by forecasting eligibility and documentation requirements before requests are submitted. This reduces delays, minimizes claim denials, and removes a major source of frustration for both clinicians and administrative staff.
When predictive intelligence is embedded into daily workflows, clinicians spend less time validating data and more time practicing medicine. Over time, this leads to improved staff retention, better patient satisfaction, and more resilient care delivery models.
Predictive Care in a 500-Bed Hospital
Consider a 500-bed multi-specialty hospital implementing ai-driven predictive care in healthcare across inpatient and outpatient services.
Within weeks, the system integrates EHR data, bedside monitoring, imaging results, and patient-reported outcomes. Agentic AI models continuously assess risk profiles for every admitted patient.
A medical ward begins to see the impact first. Patients at risk of sepsis are identified 24 to 36 hours earlier than before. Care teams receive actionable insights rather than generic alerts, enabling early diagnosis and timely intervention.
In cardiology, AI-based patient outcome forecasting adjusts medication plans based on predicted readmission risk. In oncology, care personalization improves by aligning treatment protocols with individual response patterns.
Operationally, staffing schedules are optimized based on predicted patient acuity. Automated prior authorizations reduce discharge delays. Over six months, the hospital sees measurable outcomes, including reduced length of stay, fewer adverse events, and improved clinician satisfaction.
Similar innovation pilots are already emerging in health-tech ecosystems such as Hyderabad, where hospitals and digital health partners collaborate to operationalize predictive intelligence at scale.
Governance, Trust, and Clinical Confidence in Predictive Systems
Adopting predictive care is not just a technology decision. It is a governance decision.
In 2026, trust in AI systems is built through transparency, validation, and clinical oversight. Leading organizations ensure that predictive models are explainable, regularly audited, and aligned with regulatory requirements. Clinicians remain in control, with AI serving as a decision support partner rather than an autonomous authority.
This balance between automation and human expertise is what makes predictive care sustainable and ethically sound.
Conclusion
In 2026, the shift from reactive to proactive care is no longer theoretical. It is a strategic imperative for healthcare organizations that want to deliver better outcomes while maintaining operational resilience.
By embedding ai-driven predictive care in healthcare, hospitals unlock early diagnosis, care personalization, and clinician-focused decision support that scales across departments. These systems transform data into foresight and foresight into action.
Organizations partnering with an experienced AI development company in Hyderabad gain the technical depth and healthcare expertise required to operationalize this vision.
Theta Technolabs brings proven capabilities across Web, Mobile and Cloud platforms, enabling healthcare providers to build secure, scalable predictive care ecosystems aligned with real-world clinical needs.
Explore Proactive Care Implementation
If you are exploring how predictive intelligence can be implemented across your clinical and operational workflows in 2026, now is the time to take a practical next step.
Connect with the healthcare AI specialists at Theta Technolabs at sales@thetatechnolabs.com to discuss a tailored roadmap for deploying agentic AI, healthcare predictive analytics, and outcome forecasting solutions within your organization.
Frequently Asked Questions
How is ai-driven predictive care in healthcare different from traditional analytics? Traditional analytics focuses on historical reporting and detection. Predictive care forecasts future risks and outcomes, enabling proactive intervention.
Can predictive systems integrate with existing hospital infrastructure?
Yes. Modern platforms are designed to integrate with EHRs, monitoring devices, and operational systems without requiring full replacements.
Does AI replace clinical judgment?
No. AI augments clinical decision support by providing insights, while clinicians retain final authority over care decisions.
What data is required to implement predictive care?
Most systems leverage existing clinical, operational, and patient-generated data, enriched with real-time signals for continuous learning.
How quickly can hospitals see results?
Many organizations observe measurable improvements within three to six months of deployment, depending on scope and maturity.

















_Computer%20Vision-enabled%20Web%20and%20Mobile%20Interfaces%20for%20Mall%20Management%20in%20Dubai_Q1_In_24.avif)
_Smart%20Solutions%20for%20Healthcare_%20How%20IoT%20Development%20is%20Reshaping%20Dubai%20Hospitals_Q1_In_24.avif)
_Automated%20Checkout%20Systems.avif)
_Smart%20Manufacturing%20in%20Dubai_%20How%20AI%20is%20Driving%20Efficiency%20and%20Innovation_Q1_In_24.avif)

_Understanding%20the%20Impact%20of%20AI%20and%20Machine%20Learning%20on%20Fintech%20Web%20Apps%20in%20Dubai_Q2_24.avif)
_Explore%20the%20Best%20Cross-Platform%20App%20Development%20Frameworks%20of%202024_Q3_24.avif)


_Top%20Benefits%20of%20Cloud%20Computing%20for%20All%20Business%20Sectors_Q2_24.avif)
_Integrating%20IoT%20with%20Mobile%20Apps%20for%20Advanced%20Renewable%20Energy%20Solutions_Q2_24.avif)


_The%20Transformative%20Role%20of%20Open%20Banking%20APIs%20in%20Fintech%20for%202024_Q3_24.avif)
_Choosing%20the%20Right%20Computer%20Vision%20Development%20Partner%20in%20Ahmedabad%20for%20Construction_Q3_24.avif)
_Node.js%20and%20Blockchain_%20A%20Perfect%20Pair%20for%20Fintech%20Innovation%20in%20Dubai_Q3_24.avif)
_How%20AI%20Development%20Companies%20in%20Ahmedabad%20are%20Transforming%20the%20Shopping%20Experience_Q4_25.avif)
_How%20IoT%20Can%20Reduce%20Energy%20Costs%20in%20Smart%20Factories_Q4_25.avif)























.avif)
.avif)
.avif)


































.png)




.png)

















